1. It's not just in the stomach: the symptoms go far beyond the intestines
Although abdominal pain, bloating, and changes in bowel habits are the core symptoms of IBS, its manifestations can spread throughout the body in ways that many wouldn’t associate with a digestive problem. This condition reveals how interconnected the systems of the human body are.
Many patients with IBS also report extraintestinal symptoms that significantly affect their overall well-being. Among the most common are:
- Lower back pain
- Headaches
- Fatigue
- Decreased vitality
This demonstrates the importance of looking at the body as a whole. Symptoms are not confined to a single organ; they are signs of a broader imbalance involving multiple systems communicating with each other.
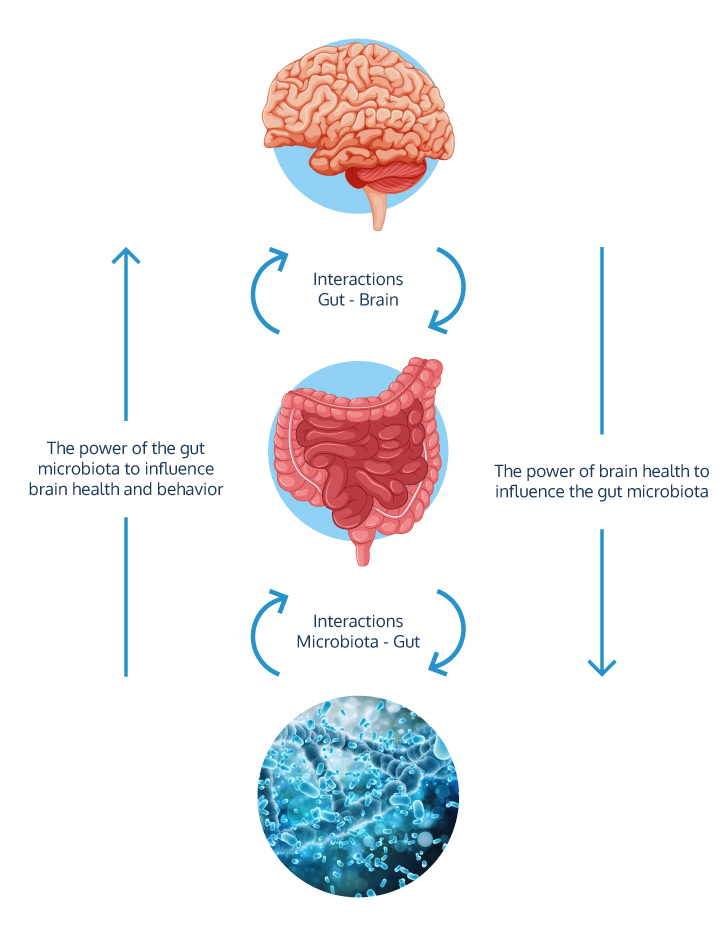
2. The brain as the "conductor" of pain
One of the most transformative concepts in understanding IBS is the central role of the brain-gut axis. Although triggers may originate in the gut, the experience of pain is ultimately a creation of the brain.
Science is clear on this point: regardless of the initial triggers of the symptoms, “the brain is ultimately responsible for constructing and generating the conscious perception of abdominal pain, discomfort, and anxiety based on sensory information from the gut.”
This changes everything. It means that pain is not just damage to the intestinal tissue, but an interpretation by the brain. That’s why emotional state doesn’t just “worsen” symptoms – it’s an integral part of the mechanism that creates them. But how does the brain receive these messages from the gut? Through an information “superhighway.”
3. The secret "highway" that connects everything: the vagus nerve
If the brain and gut are in constant communication, what pathway do they use? The main pathway is the vagus nerve, a crucial component of our nervous system that acts as the primary “modulator” of the brain-gut-microbiome communication pathway.
Its nerve endings in the intestines establish a direct connection with the enteric nervous system (the “brain” of the gut). This nerve is activated by microbes and the metabolites they produce, which are directly influenced by diet, helping to generate functional digestion patterns.
Any alteration in this complex communication pathway, whether in the brain, the nerve itself, or the intestinal ecosystem, is implicated in the pathophysiology of IBS. And one of the factors that can most disrupt the “traffic on this highway” is stress, which has the power to reshape the very starting point of communication: the intestinal ecosystem.
4. Stress physically alters the gut ecosystem
The idea that stress can alter the stomach is more literal than you think. Psychosocial factors have a direct and measurable impact on the ecosystem of bacteria that lives in the human gut, a phenomenon known as dysbiosis.
The research confirms that “there is scientific evidence regarding the psychosocial effect on the abundance of gut microbes.” What this means is that stress is not an ethereal emotion. It is a biological event that acts as a “bad gardener” in the gut, favoring the growth of microbial “weeds” at the expense of beneficial bacteria. This imbalance, or dysbiosis, sends constant alarm signals to the brain, perpetuating the cycle of pain and discomfort.
5. An unexpected help: osteopathy
When you understand IBS as a disorder of the brain-gut axis, and not just as a digestive problem, new therapeutic approaches begin to make sense. In addition to diet and psychotherapy, osteopathy emerges as a surprising, yet logical, option.
When you understand IBS as a disorder of the brain-gut axis, and not just as a digestive problem, new therapeutic approaches begin to make sense. In addition to diet and psychotherapy, osteopathy emerges as a surprising, yet logical, option.
- Adjustment of the Polygon of Forces, adjusting the body's tensor apparatus and its mechanical-physiological relationships in the abdominal and pelvic cavity and its relationships with the vertebral central arch and baseline.
- Fascial release of structures such as the small intestine, colon, root of the mesentery, and greater omentum, to restore mobility and physiological motility.
- Diaphragmatic work: Addresses the fascial relationship of the diaphragm with the visceral structures and its insertion (pillars D11-L3), crucial for managing internal pressure.
- Cranial techniques and suboccipital decompression: These aim to directly influence the vagus nerve, helping to "calm" the communication pathway and promote a state of greater relaxation and digestive function (parasympathetic).
This integrative approach reflects the philosophy of osteopathy, as mentioned by John Wernham:
“There is only one Osteopathy and that only way is through the process of INTEGRATION”
Conclusion: The Body Speaks in Unison
Irritable Bowel Syndrome (IBS) is a perfect example of how the body doesn’t function in isolated parts. It’s a deeply integrated system where digestive health, the nervous system, and emotional state are intrinsically linked. Understanding these connections not only demystifies the condition but also opens doors to more holistic and effective therapeutic approaches.
After seeing these connections, do we hear all the messages that the body is trying to send us?